Brain vasculature system
Our goal is to understand the principles underlying the formation of the brain vasculature system. Brain endothelial cells (ECs) are one of the major components of brain vasculature system and involved in many kinds of genetic diseases and neuroninflammation related diseases, like bAVM, CCM, HHT, IA (Intracranial aneurysm), multiple sclerosis (MS) and stroke. We are developing and applying cutting edge technologies to interrogate the signal transduction pathways that involved in disease progression.
One the road of discover new molecular machinery that governs the functions of brain endothelial cells……
I. To understand the molecular basis of physiological process of brain endothelial cells
 Our goal is to understand the principles underlying the formation of the brain vasculature system. Brain endothelial cells (ECs) are one of the major components of brain vasculature system and involved in many kinds of genetic diseases and neuroninflammation related diseases, like bAVM, CCM, HHT, IA (Intracranial aneurysm), multiple sclerosis (MS) and stroke. We are developing and applying cutting edge technologies to interrogate the signal transduction pathways that involved in disease progression.
Our goal is to understand the principles underlying the formation of the brain vasculature system. Brain endothelial cells (ECs) are one of the major components of brain vasculature system and involved in many kinds of genetic diseases and neuroninflammation related diseases, like bAVM, CCM, HHT, IA (Intracranial aneurysm), multiple sclerosis (MS) and stroke. We are developing and applying cutting edge technologies to interrogate the signal transduction pathways that involved in disease progression.
Q1. How is BBB Permeability dynamically regulated in health or disease state ?
Q2. What are the molecular machineries that mediate transcytosis and how do they work cooperatively ?
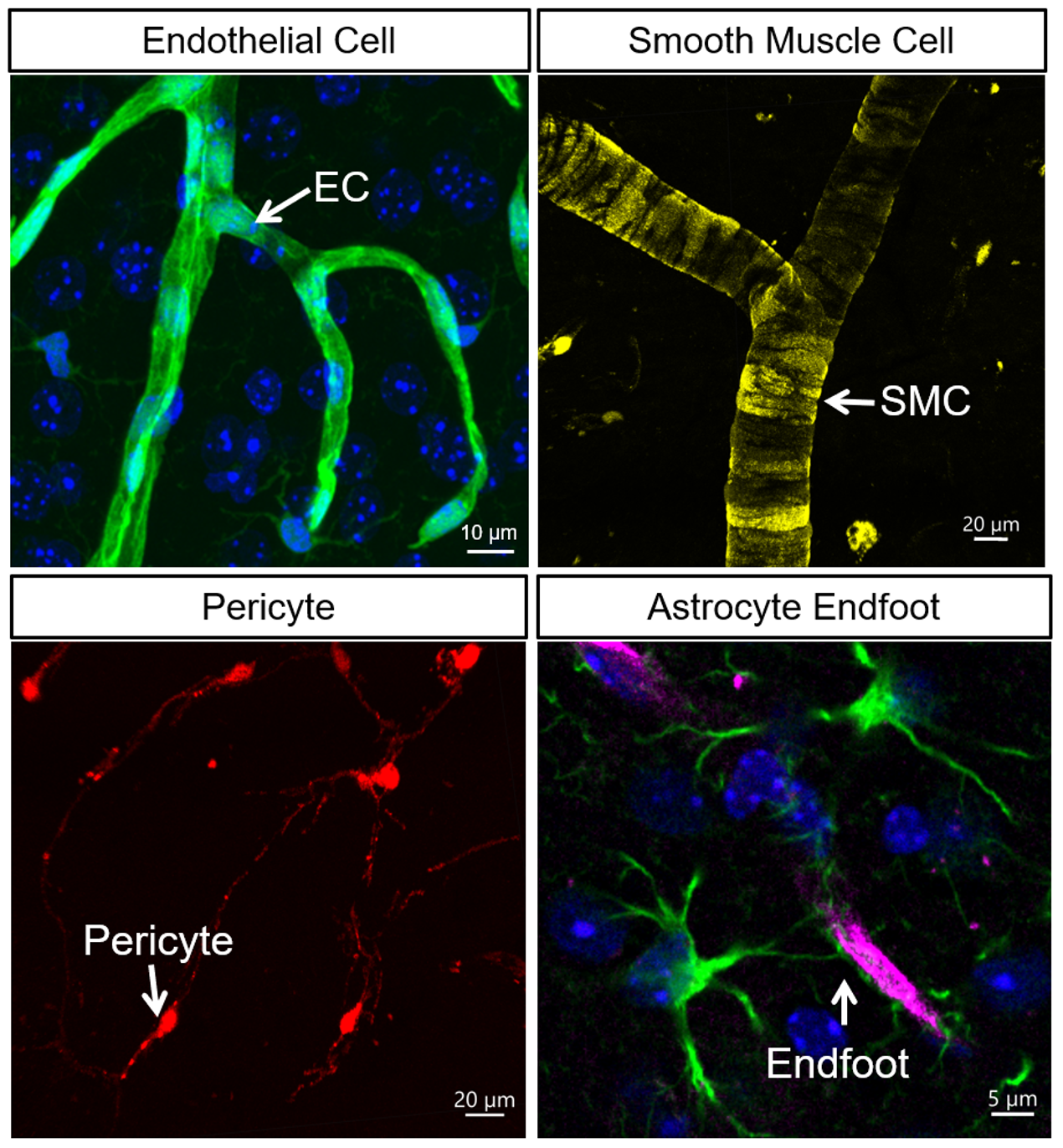 Early anatomical and cytological studies established the basic cellular composition of the brain’s vascular system, including smooth muscle cells (SMCs) on arteries, pericytes on capillary walls, and endothelial cells (ECs) as the fundamental component. Additionally, astrocytic endfeet envelop the perivascular space around the vessel walls. Parenchymal glial cells and neuronal cell bodies are also found in close proximity to cerebral vessels, typically within 15 μm.
Early anatomical and cytological studies established the basic cellular composition of the brain’s vascular system, including smooth muscle cells (SMCs) on arteries, pericytes on capillary walls, and endothelial cells (ECs) as the fundamental component. Additionally, astrocytic endfeet envelop the perivascular space around the vessel walls. Parenchymal glial cells and neuronal cell bodies are also found in close proximity to cerebral vessels, typically within 15 μm.
In order to target brainECs, we decided to create following genetic tools.
1. Development of a brainEC specific Cre driver line: Slco1c1-CreER-KI
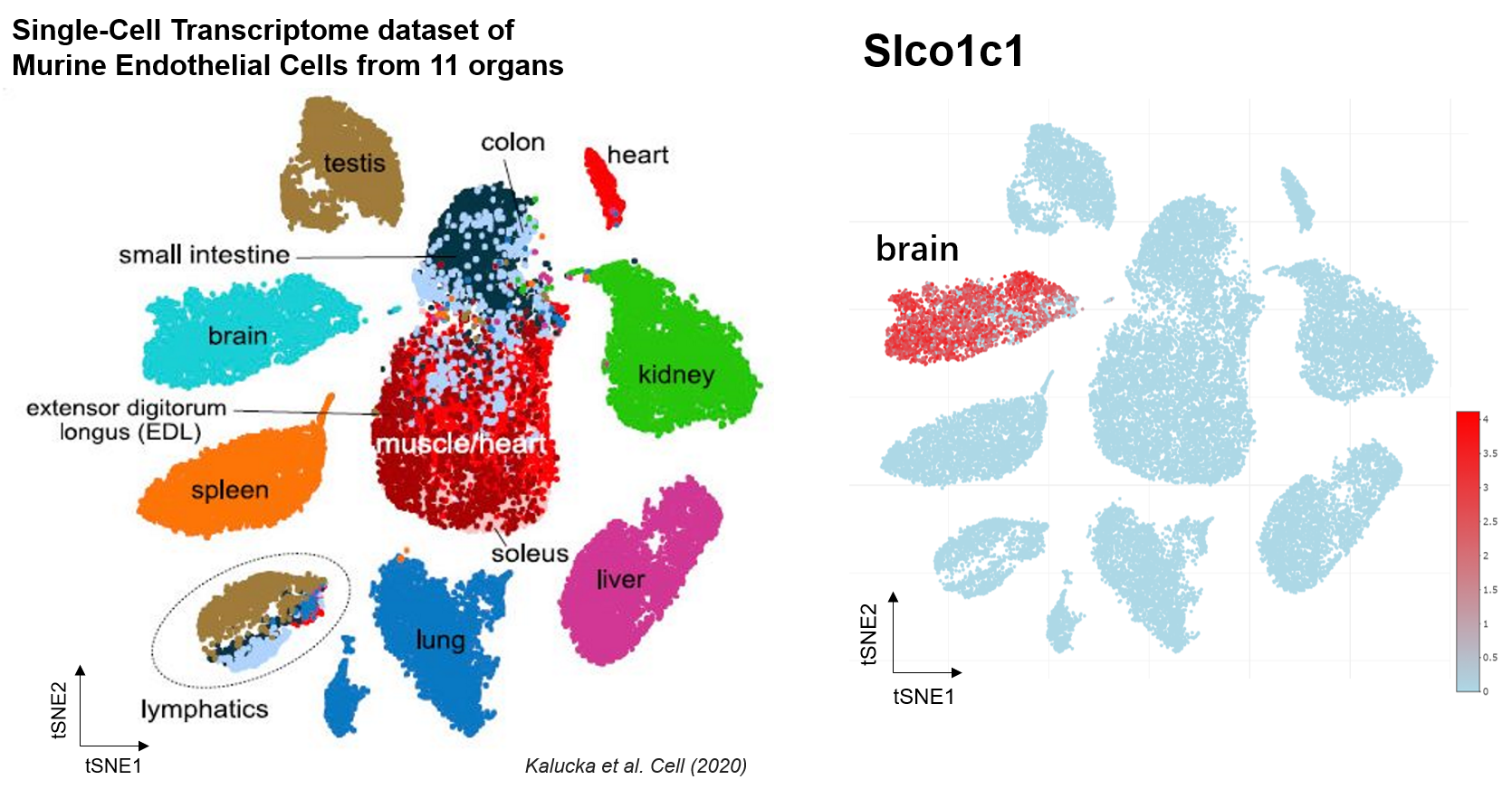
Slco1c1 gene is restricted expressed in endothelial cells in central nervous system (CNS). Slco1c1 transporter mediates the Na(+)-independent high affinity transport of organic anions such as the thyroid hormones L-thyroxine (T4), L-thyroxine sulfate (T4S), and 3,3’,5’-triiodo-L-thyronine (reverse T3, rT3) at the plasma membrane.
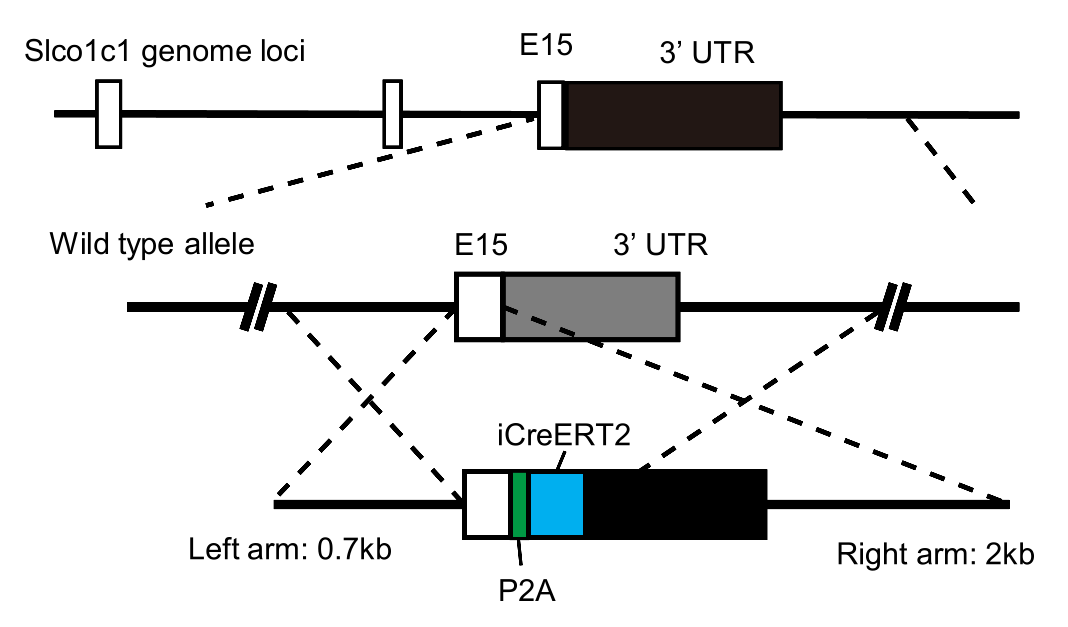
A schematic showing the strategy used to develop the Slco1c1-CreER-KI mouse line.
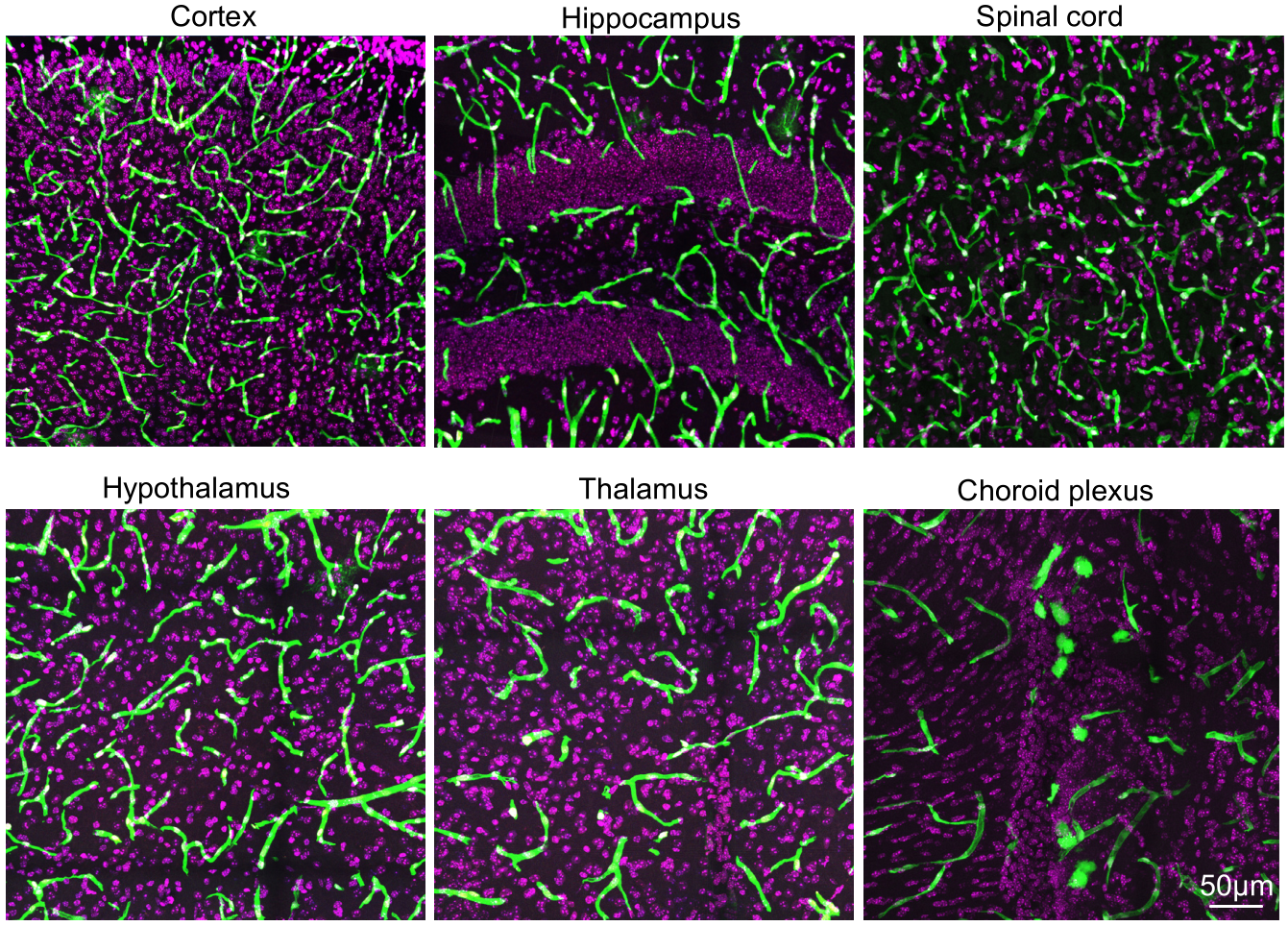
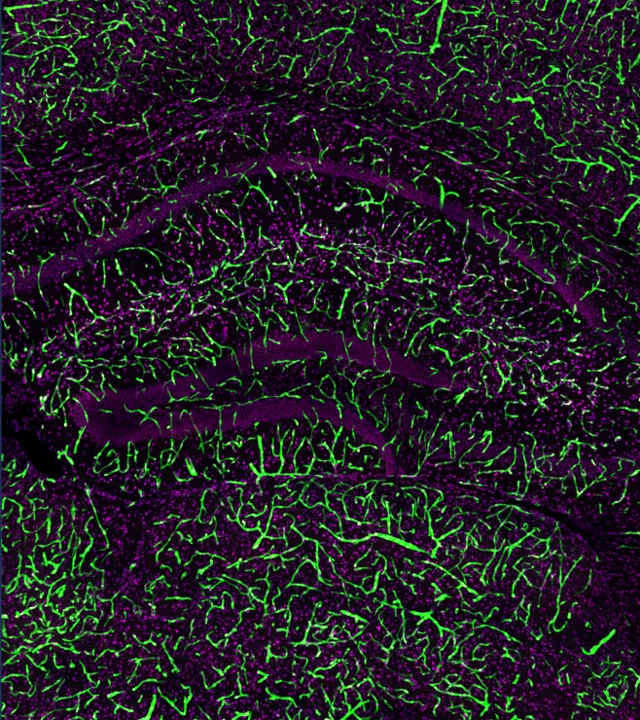
The expression pattern of EGFP in different brain regions of Slco1c1-CreER-KI :: Ai47 mice. EGFP, green; Nuclei, DAPI (purple).
2. Development of rAAV-miniBEND system, A targeted vector for brain endothelial cell gene delivery and gene therapy
Application 1. rAAV-miniBEND enable highly efficient labeling of Rat brainECs and retina ECs.
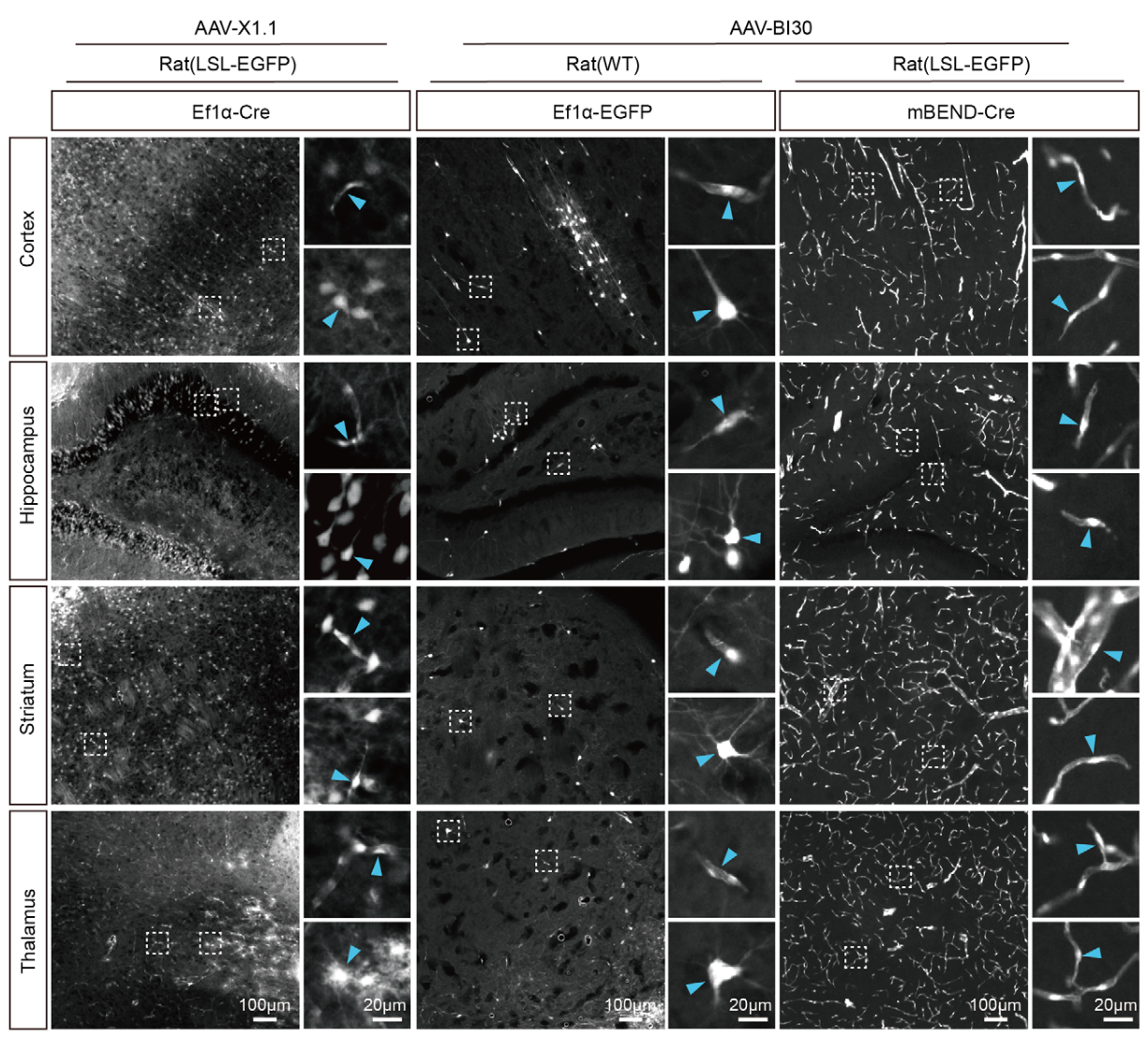
The rAAV-miniBEND system facilitates highly efficient gene delivery to rat brainECs through retro-orbital injection. Representative images showing the endothelial labeling efficiency and specificity in various brain regions at PID21 following injection with AAV-X1.1-Ef1α-Cre, AAV-BI30-Ef1α-EGFP, or AAV-BI30-miniBEND (mPro723-mCis700)-Cre into both wild-type (WT) rats and the transgenic strain Rosa26-CAG-LSL-EGFP.
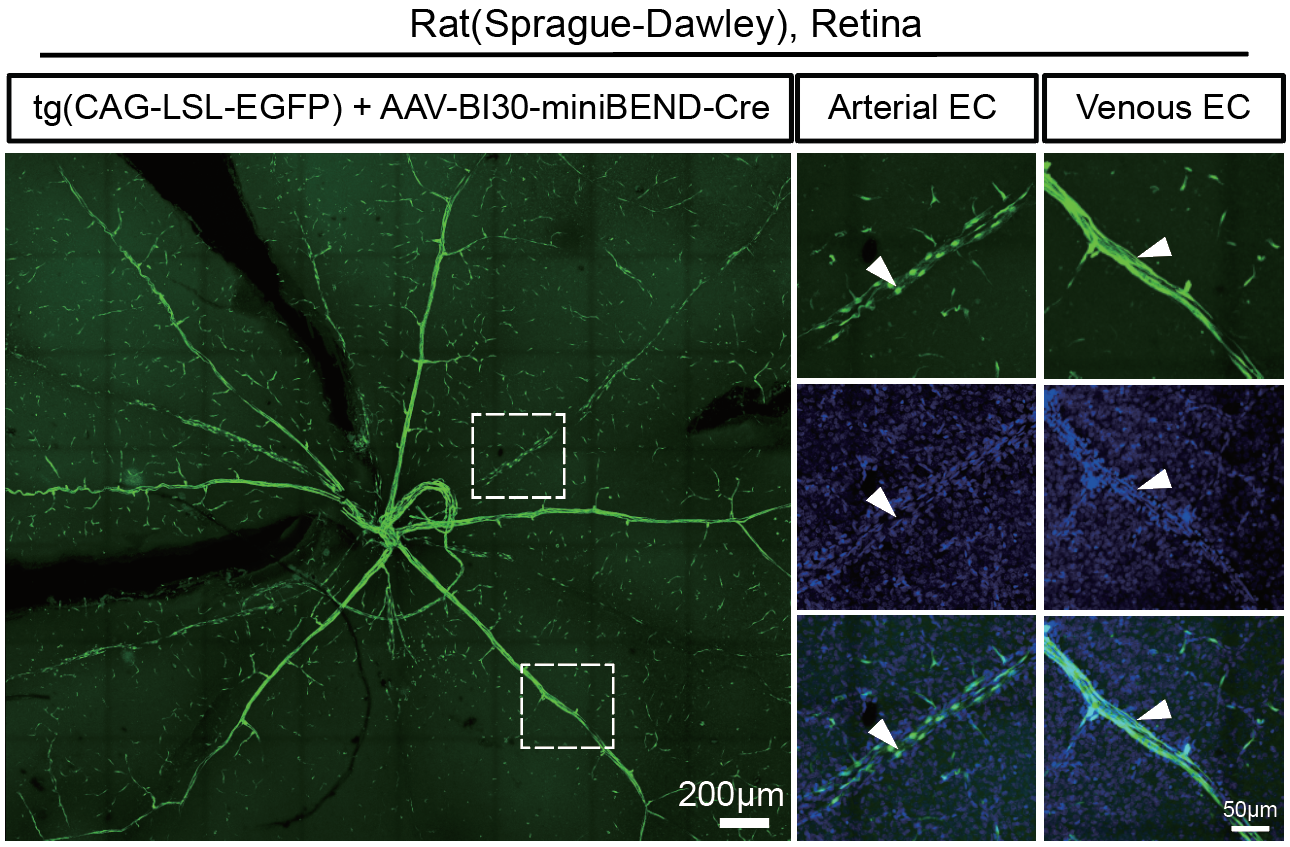
Representative images of retinas were captured at 21 days after retro-orbital injection of AAV-BI30 for gene delivery to retinal vascular endothelial cells in P3 rats. Specifically, AAV-BI30-miniBEND-Cre virus (AAV-BI30-mPro723-Cre-mCis700) was injected into transgenic rats (Rosa26-CAG-LSL-EGFP). The white arrowheads indicate vascular endothelial cells (right panel).
Application 2. somatic genetic analysis of the brainECs.
Aim 3. Targeted delivery of brainECs in Non-human Primates (NHPs).
Aim 4. Development of gene therapy products for clinical usage.
One the road of curing diseases by creating tools and drugs……
One the road of hunting new disease target and drug target……
II. To dissect signaling pathway that control the pathogenesis of CCM disease
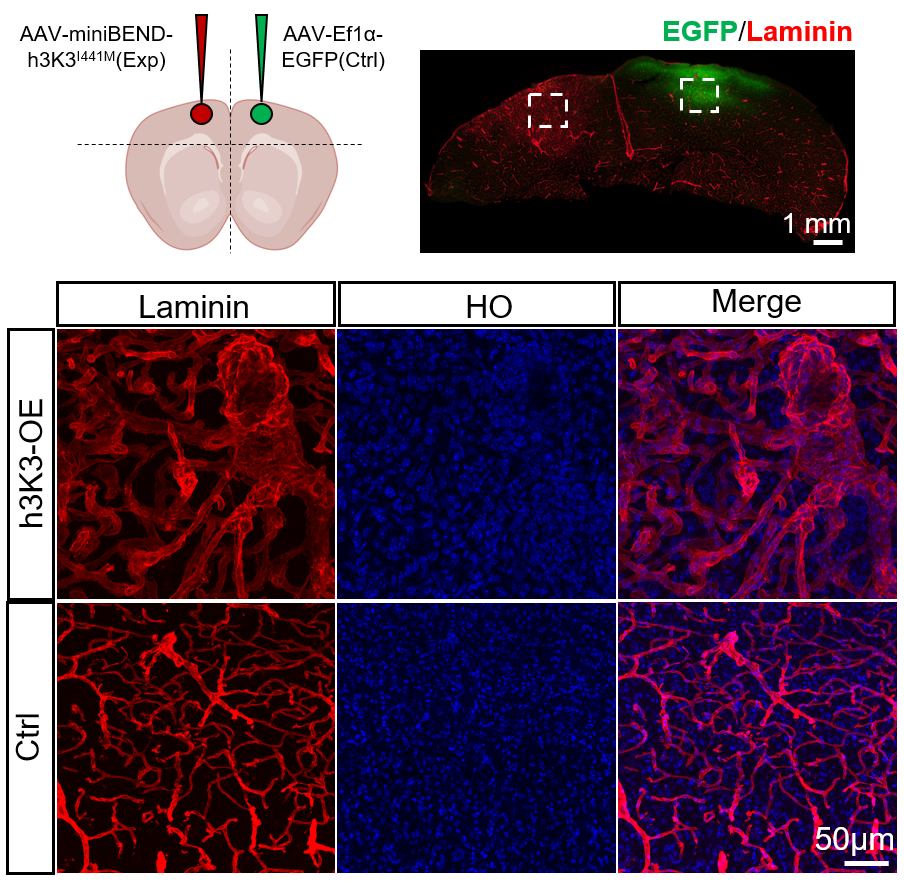
1. Somatic activation of MAP3K3 signaling in brainECs is sufficient to cause cerebral cavernous malformations (CCM).
Next questions
Q1. How MAP3K3 kinase activity is regulated by CCM complex ?
Q2. What is the downstream effctor that lead to CCM vascular malformation ?
III. To dissect signaling pathway that control the pathogenesis of bAVM disease
1. Activation of BRAF-MEK1 signaling pathway is sufficient to trigger brain arteriovenous malformations (bAVM).
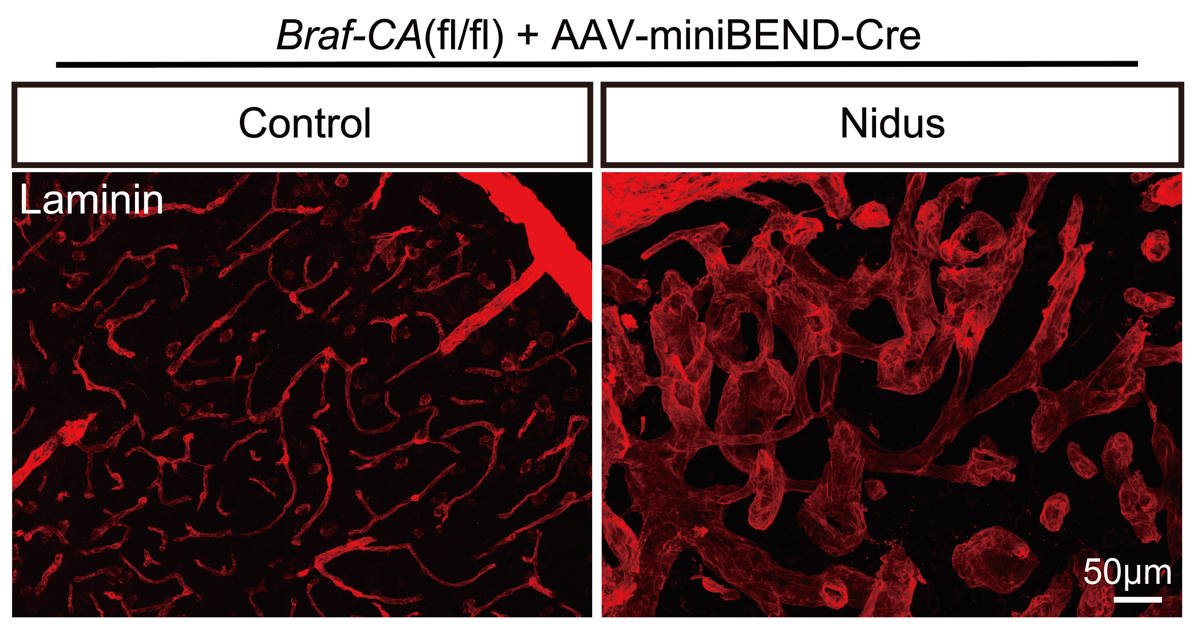 We firstly prove that Braf is a disease causing gene for brain arteriovenous malformations (bAVM) disease by providing comprehensive evidences (Li et al., 2025).
We firstly prove that Braf is a disease causing gene for brain arteriovenous malformations (bAVM) disease by providing comprehensive evidences (Li et al., 2025).
Next questions
Q1. What are the negative regulators that prevent the initiation of bAVM vascular malformation ?
IV. To explore and characterize the role of bECs in inflammatory response
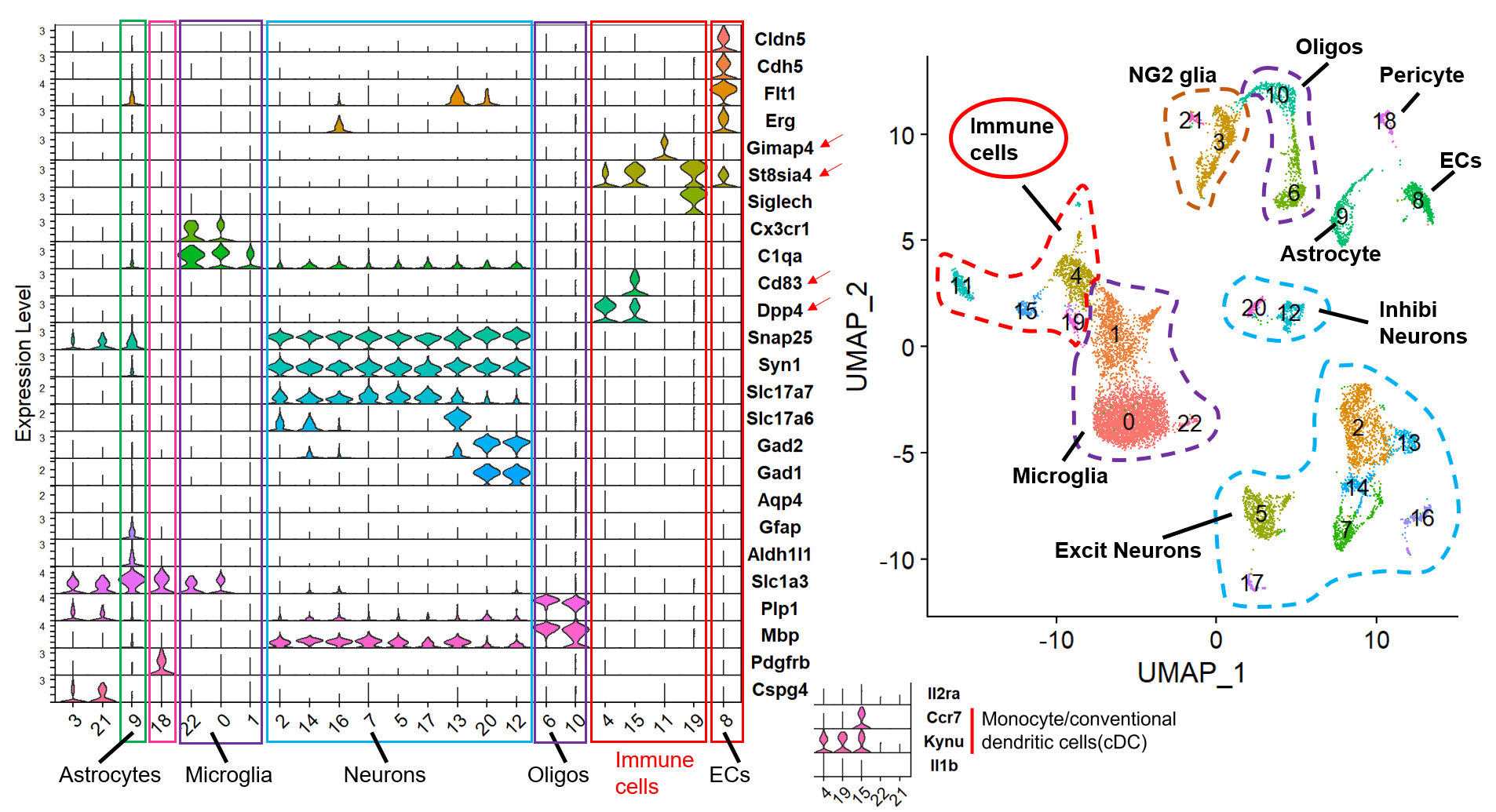
Immune cell infiltration revealed by snRNAseq of bAVM lesion
We characterized that monocyte and conventional dendritic cells (cDCs) are the main immune cell types that infiltrate in bAVM lesion. We also observed inflammation-mediated angiogenesis in bAVM lesion. And, Ackr1 gene is significantly upregulated during early stage of bAVM (Li et al., 2025). Ackr1 gene encodes the atypical chemokine receptor 1 (ACKR1, a.k.a. CD234, also known as the Duffy antigen receptor for chemokines (DARC)). This chemokine receptor is primarily expressed by postcapillary venules (PCV) ECs (and small venule ECs) (Thiriot et al., 2017), and transports basal chemokines for presentation at the luminal surface of ECs and in paracellular junctions, where it regulates different stages of immune cell diapedesis (Girbl et al., 2018) and recruitment (Girbl et al., 2013).
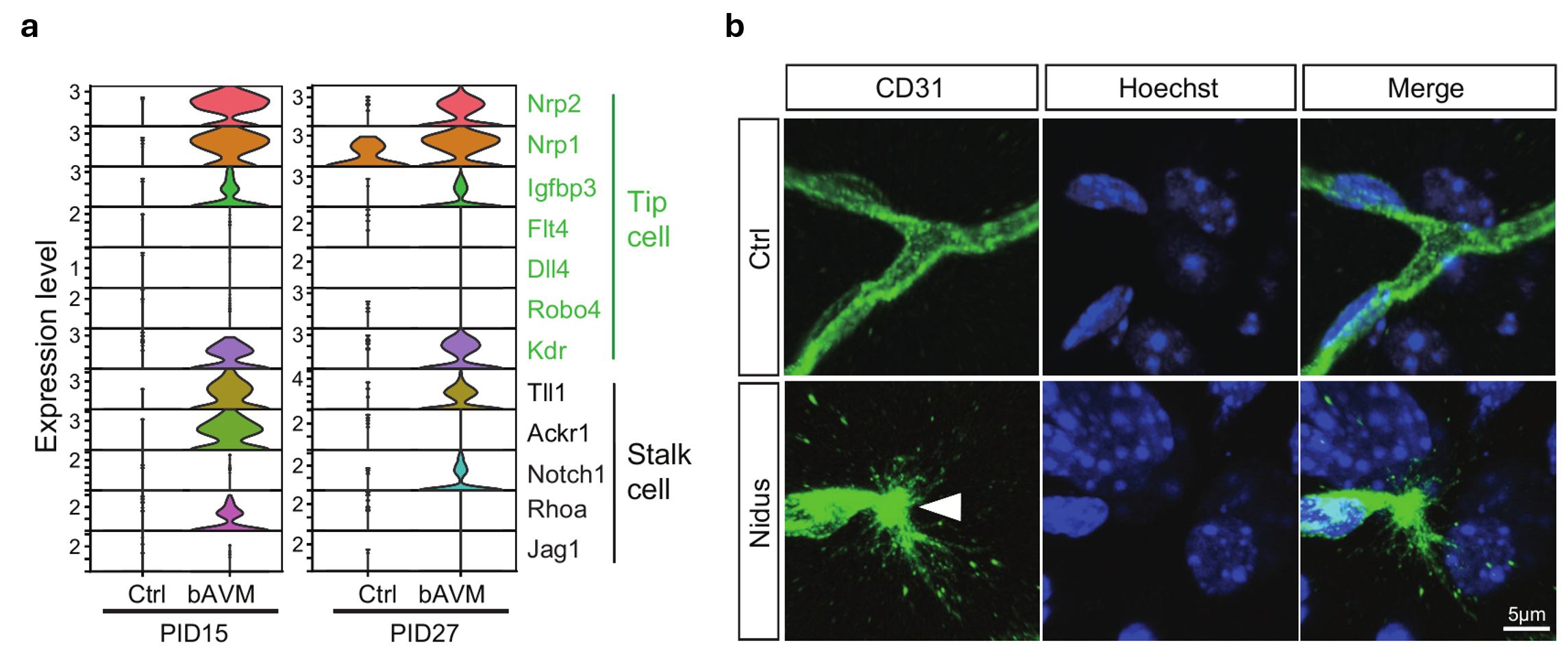
(a) Marker genes related to tip and stalk cells in endothelial cell clusters among DEGs from both early (PID15) and late (PID27) developmental stages of AVMs. (b) Representative image of an individual tip cell in the bAVM lesion area. White arrowhead, a filopodia from the tip cell; green, anti-CD31; blue, nuclei (Hoechst 33342).
Next questions
Q1. How inflammation signaling promote the progress of bAVM disease ?
Other questions
Q1. The mechanisms of BBB disruption during inflammatory conditions of multiple sclerosis remain poorly defined.
Q2. What is the molecular basis of vascular regression in the aging brain ?
While the intervascular connective tissue strands in the central nervous system (also named string vessel or acellular capillaries) have been observed and documented for decades (Cammermeyer 1960; Brown et al., 2010). its underlying cellular and molecular mechanisms remain largely unknown. A central, unresolved question is how these structures form.
Neuroinflammation, a hallmark of brain aging and neurodegenerative diseases, provides a compelling candidate mechanism. Driven by activated microglia and astrocytes, neuroinflammation generates a persistent stream of pro-inflammatory cytokines and damage-associated molecular patterns (DAMPs) in the brain. Consistent with this, we previously demonstrated that both brain aging and acute inflammation induced by systemic lipopolysaccharide (LPS) cause significant increase in vessel regression throughout the adult brain (Gao et al., 2020). While a recent study proposed that endothelial activation of GSDMD mediates inflammatory blood-brain barrier (BBB) breakdown (Wei et al., 2024), its specific contribution to the macroscopic process of vessel regression and string vessel formation remains uncharacterized.
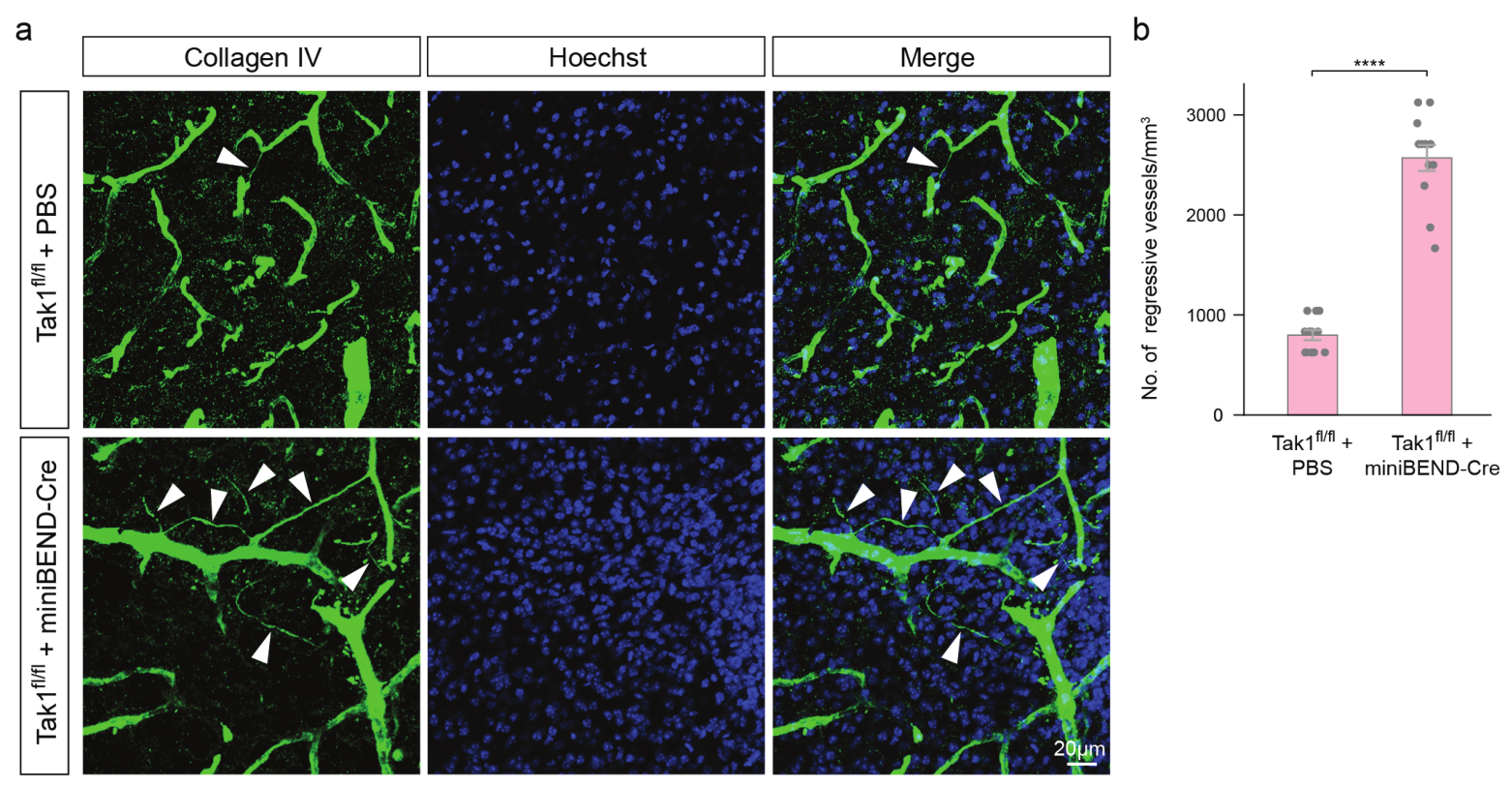
Pattern of regressive blood vessels in Tak1-fl/fl mice infected with AAV-PHP.eB-miniBEND-Cre.
a, b, Representative images (a) and a summary of the density (b) of regressive blood vessels (arrowheads) in Tak1-fl/fl mice after administration of PBS (top row, a) or AAV-PHP.eB-miniBEND (mPro723-mCis700)-Cre (bottom row, a). Unpaired two-sided Welch’s t-test; ****p < 0.0001.
Our findings demonstrate that genetic ablation of TAK1 signaling significantly increases vessel regression in the adult brain (Gao et al., 2025; Li et al., 2025). This observation is particularly intriguing given that TAK1 serves as a critical nexus in cell death signaling. In immune cells, TAK1 inhibition can lead to the activation of Caspase-8, which subsequently executes pyroptosis by directly cleaving key effectors, Gasdermin D (GSDMD) and Gasdermin E (GSDME) (Guo et al., 2016; Orning et al., 2018). Although a clear link between TAK1 and distinct cell death pathways has been established, the precise mechanisms governing these processes in brain endothelial cells remain to be elucidated. It is currently unclear whether necroptosis or pyroptosis is the dominant form of regulated cell death in these cells and, crucially, how its specific regulation contributes to the breakdown of blood-brain barrier.
Building on those evidences, we propose a framework in which the canonical TAK1–Caspase-8–Gasdermin axis, a well-defined cell death pathway in immune cells, is co-opted to drive brain endothelial cell death and subsequent vascular pathology in the context of neuroinflammation and aging. To address this critical knowledge gap, we now investigate the novel mechanisms by which dysregulated innate immunity in aging drives the structural degradation of the cerebral microvasculature.
Representative works
-
Jun-Liszt Li# ¶, Zhanying Bi#, Xingjun Chen#, Tianyue Ming, Baoshan Qiu, Fengzhi Li, Ziyan Feng, Daosheng Ai, Tingting Zhang, Jiayu Wang, Shuai Lin, Yiping Lu, Hu Zhao, Zhanjing Wang, Juan Huang, Fei Zhao, Hu Zhao, Yilong Wang, Wenzhi Sun✝, Woo-ping Ge✝. “rAAV-miniBEND: A targeted vector for brain endothelial cell gene delivery and cerebrovascular malformation modeling” Nature Biomedical Engineering (29/10/2025) [PDF | PMID: 41162685 | DOI Link] First author
- Pre-print version: BioRxiv (15/06/2025) [DOI Link]
- Conceived and lead whole project
-
Xiaofei Gao#, Xing-jun Chen#, Meng Ye, Jun-Liszt Li ¶, Nannan Lu, Di Yao, Bo Ci, Fei Chen, Lijun Zheng, Yating Yi, Shiwen Zhang, Zhanying Bi, Xinwei Gao, Yuanlei Yue, Tingbo Li, Jiafu Lin, Ying-Chao Shi, Kaibin Shi, Nicholas E. Propson, Yubin Huang, Katherine Poinsatte, Zhaohuan Zhang, Dale B. Bosco, Shi-bing Yang, Ralf H. Adams, Volkhard Lindner, Fen Huang, Long-Jun Wu, Hui Zheng, Simon Hippenmeyer, Ann M. Stowe, Bo Peng, Marta Margeta, Qingchun Guo, Xiaoqun Wang, Qiang Liu, Jakob Körbelin, Martin Trepel, Hui Lu, Guoen Cai, Bo O. Zhou, Bo Shen, Ying-mei Lu, Wenzhi Sun, Jie-Min Jia, Feng Han, Hu Zhao, Robert M. Bachoo & Woo-ping Ge* (01/07/2025) Reduction of neuronal activity mediated by blood-vessel regression in the brain. Nature Communications [PDF | PMID: 40595484 | DOI Link]
- Pre-print version: BioRxiv (15/09/2020) [DIO Link]
- Design and Characterization of a brainEC specific Cre driver line: Slco1c1-KI-P2A-iCreERT2
-
Jian Ren#, Yazi Huang#, Yeqing Ren#, Tianqi Tu, Baoshan Qiu, Daosheng Ai, Zhanying Bi, Xue Bai, Fengzhi Li, Jun-Liszt Li ¶, Xing-jun Chen, Ziyan Feng, Zongpei Guo, Jianfeng Lei, An Tian, Ziwei Cui, Volkhard Lindner, Ralf H Adams, Yibo Wang, Fei Zhao, Jakob Körbelin, Wenzhi Sun, Yilong Wang, Hongqi Zhang, Tao Hong✝, Woo-ping Ge✝ (30/03/2023) Somatic variants of MAP3K3 are sufficient to cause cerebral and spinal cord cavernous malformations. Brain [PDF | PMID: 36995941 | DOI Link]
